Does this sound like you?
You’ve been ill with an autoimmune disease for a while, but you can’t recall a battle with Epstein-Barr virus, and none of the usual triggers ring true with you, or you have worked through the ones you had and aren’t seeing the results you expect. Another seemingly unrelated health issue is that despite brushing and flossing twice a day, following with mouthwash, your dentist is not happy with your oral health. You visit her regularly only to get more bad news about the spread of gum disease or the need for a root canal. An added worry on top of your autoimmunity issues!
What if your poor oral health was the trigger for your autoimmune disease?
We can’t blame your dentist or doctor for not spotting the connection. The trouble may lie in western medicine’s continued focus on treating the mouth separately to the rest of the body – but we’re beginning to catch up. There is increased focus on the importance of oral-systemic health.
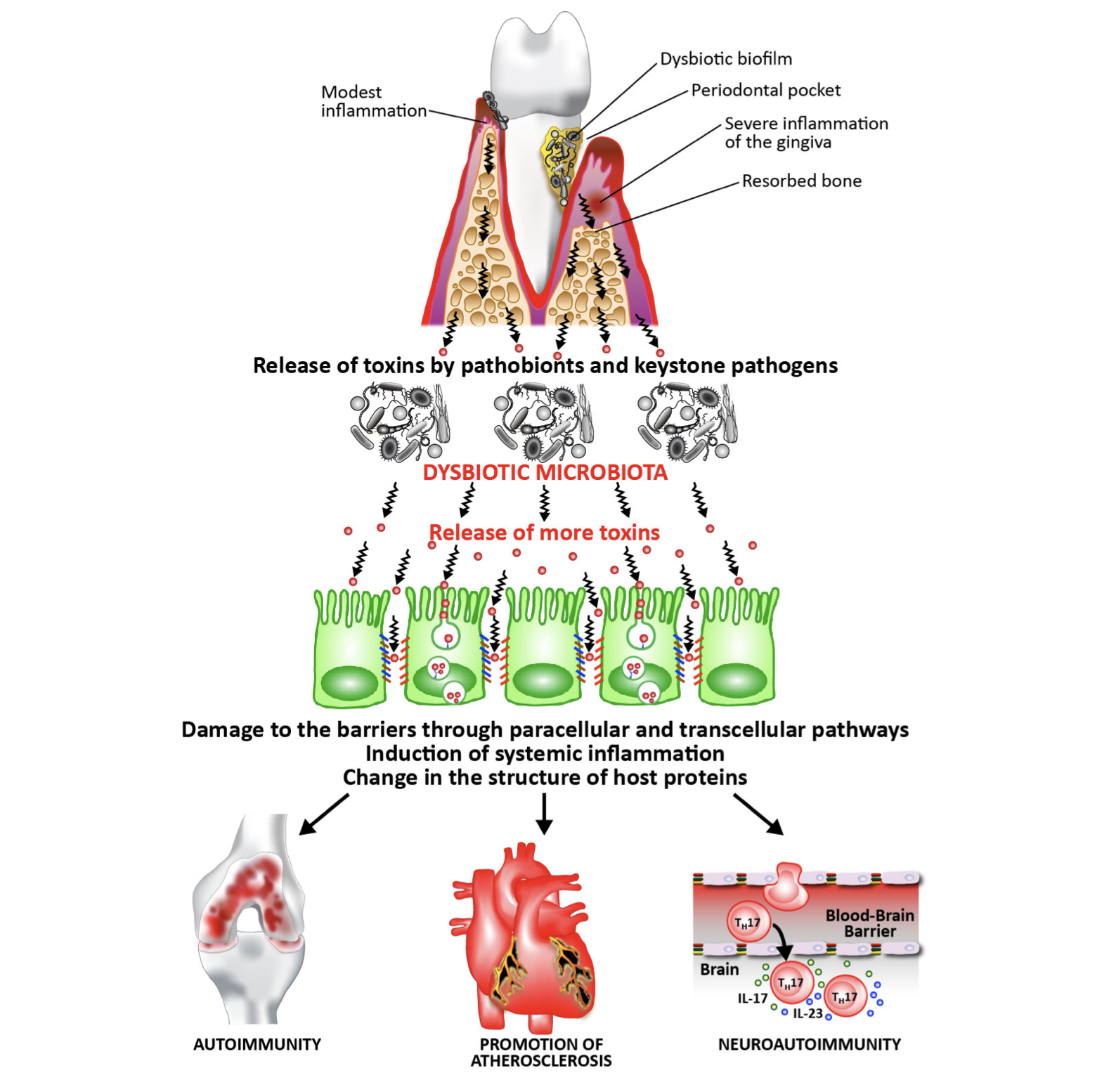
The mouth is an important gateway to the rest of your body, and often the first line of defence in regards to inflammation and the autoimmune response. It is a heavily vascular area, meaning that any toxins or bacteria getting past its defences can travel around the body quickly, causing damage and instigating an autoimmune response.
There are over 100 diseases of the body originating in the mouth.
Is your autoimmune disorder one of them?
What Is the Oral Microbiome?
The oral microbiome cannot be seen, but it’s one of the most fascinating parts of the inside of your mouth. Your mouth is warm, moist, full of food particles – the perfect place for microorganisms to thrive – and that’s a good thing! Your oral microbiome behaves similarly to your gut microbiome – the ‘good’ bacteria keeps the ‘bad’ bacteria in check. The bacteria feed on food debris from your chewing.
Your oral microbiome is made up of similar bacteria to that in your gut, which adheres to your teeth as a biofilm. Biofilms are made up of communities of bacteria interlinked and able to communicate and collaborate with each other to build up resistance to your immune system.
When your mouth is healthy, the good microorganisms work together to contribute to your body’s workings in the following ways:
- Digesting food debris
- Generating energy
- Colonisation resistance
- Maturing epithelium cells and maintaining mucosal barriers (basically, maintaining a healthy environment by doing structural maintenance)
When your oral microbiome misbehaves, it initially causes mild diseases of the mouth, which can be treated by a dentist. However, an oral disease can trigger an autoimmune disease in susceptible individuals and can perpetuate it in others.
When Your Oral Microbiome Goes Wrong
When you’re healthy, the makeup of your oral microbiome remains stable. However, eating large quantities of refined sugar, having poor saliva levels, or maintaining poor oral hygiene can affect your oral microbiome for the worse. Dental implants, bridgework and prosthetics can all disrupt your oral microbiome, as the microorganisms are unable to stick to the man-made surfaces.
An unhealthy oral microbiome can cause:
- Dental caries or cavities – small holes in the enamel of your teeth, caused by acid secreting bacteria.
- Subgingival plaque, leading to –
- Gingivitis – more commonly known as gum disease, is the condition where your gums become sore, inflamed, or swollen. Caused by a buildup of plaque – excreted by the bad bacteria in your mouth that feeds on food debris and sugar – gingivitis is best treated before it can progress into the more serious periodontal disease.
- Periodontitis – otherwise known as periodontal disease. When you develop this disease, your gum tissue begins to pull away from your teeth and form little crevices: perfect for nasty bacteria to bed down in and multiply, causing infection.
- Pulp infection in the centre of your tooth, leading to a root canal or tooth removal.
However, the results of an unhealthy oral microbiome don’t start and end in the mouth. Due to the link between oral and systemic health, an unhealthy mouth can trigger a whole host of autoimmune issues in the rest of your body.
Periodontitis may cause a systemic anti inflammatory response and depending on your genetic and environmental predispositions can trigger:
- Poorly managed type 2 diabetes
- Cardiovascular disease, which is also an autoimmune disease
- Rheumatoid Arthritis
Remember, there are over 100 systemic diseases that begin in your mouth. Yet, most of the time, dentistry is seen as a separate field to medicine, when really the disciplines need to be tied closer together.
Lets Look More Closely at P.Gingivalis.
Porphyromonas gingivalis is part of the oral microbiome that is also closely involved with periodontal disease. But what we now know is that if you have this pathogen, you are at a much greater risk of autoimmune disease such a rheumatoid arthritis! In fact it has been shown that the severity of periodontal disease directly influences the onset of rheumatoid arthritis, and that treating it successfully reduces Rheumatoid antibodies and the severity of symptoms.
You’ve Heard of Leaky Gut, but What Is Leaky Mouth?
So, leaky gut is a condition where your intestinal permeability is affected, and your gut no longer filters the food you’ve digested correctly.
The holes in your gut wall become larger and the ‘bad stuff’, like toxins and food debris, along with the good nutrients, filter into your bloodstream unchecked.
But did you know the exact same process can happen in the mouth, too?
Leaky mouth resembles leaky gut, but – you guessed it – leaky mouth occurs in your mouth! Your gum line is an incredibly vascular area of the body that provides protection from a barrage of bacteria, toxins, and fungi. The junctional epithelium in your mouth works on the same basis as your gut wall: like a bouncer to a nightclub, admitting an approved guestlist only.
But when the epithelium is damaged by inflammation, bacteria can slip through – the doorway the bouncer has to guard is much larger, and he can’t always check the larger crowds thoroughly. Allowing bacteria, toxins, and fungi into your bloodstream can often lead to complications elsewhere in the body, triggering an aggressive autoimmune response.
An interesting example of this was reported in the journal of Clinical Pediatrics, where a patient on a gluten-free diet still exhibited signs of coeliac disease. Her retainer contained a non dietary source of gluten – a common ingredient in plastics. The gluten was being absorbed through her gums and into her bloodstream.
This example illustrates just how porous the gum line is, and, combined with the heavily vascular nature of the area, it’s no surprise that it’s so easy for the bacteria and other nasty stuff to travel through your body, with the potential to trigger other autoimmune responses.
Heavy Metals and Plastics
Oral systemic issues don’t end there. Unfortunately, man-made materials can also contribute to poor health – some of which are introduced by dentists! I touched upon the risks of glutenated plastics, but I’d like to look at dental work in more detail.
Materials to avoid when considering your systemic health include, but are not limited to:
Metals
- Mercury – Mercury is toxic, but it is currently still used in dental amalgam for fillings. The EU has voted in favour of a gradual phase down in dental amalgam, but the regulation does not help people with existing dental amalgam fillings. Some patients carry a gene that makes them more susceptible to mercury toxins – toxins that can trigger an autoimmune response, and are easily carried around the body via leaky mouth.
- Nickel – Nickel allergy is very common, but the metal is still found in many removable and non-removable dental aids.
- Mixed metals – For example, having two fillings in your mouth, one made of dental amalgam, and the other gold. A combination of different metals can result in oral galvanism, where the metals react with your saliva to create a painful electrical current! The current triggers an autoimmune response in your mouth.
Plastics
- BPA – BPA exposure can cause several endocrine disorders, including some cancers and is heavily linked to autoimmunity via multiple mechanisms.
- BPS – BPS is the alternative to BPA, often referred to as “BPA-free” but animal studies show that it is as toxic a material as BPA.
- Phthalates – used to make PVC, phthalates can leech out of retainers and cause DNA damage.
- Gluten – Gluten can be absorbed out of plastics and into the mouth, causing a reaction in sensitive individuals.
Ingredients in oral healthcare products
- Fluoride – consumption of fluoride over the daily limit can cause hypomineralization of your tooth enamel, nerve damage, and brain fog.
- Triclosan – exposure in early age can trigger autoimmune reactions, such as allergies and respiratory issues. Triclosan is a disinfectant, which suggests it has a bad effect on the oral microbiome.
- Titanium dioxide – large quantities of titanium dioxide can provoke oxidative stress, resulting in cell damage, inflammation, and an autoimmune response.
So-called “everyday” chemicals and materials can cause havoc, triggering an autoimmune response in susceptible individuals, so it’s important to be mindful of what materials you and your dentist choose to use.
Though you may be genetically more susceptible to developing an autoimmune disease, there are always ways to manage the day-to-day effect it has on your health through looking after your mouth, by:
- Selecting the right diet
- Reducing stress
- Looking after your oral hygiene
- Stopping smoking
- Not using harsh antiseptic mouthwashes and toothpastes. Try flouride free toothpaste and oil pulling with coconut oil!
- Helping your oral microbiome thrive
You can reduce the effect of your mouth as an autoimmune trigger, and improve both your oral health and general health.
Every part of your body is connected – your mouth is often overlooked, but it’s an important part, often influencing your systemic health in interesting ways. If you’re concerned, I urge you to find a functional medicine practitioner or dentist who can guide you in the right direction, towards total healing.
If you’re suffering from autoimmunity and feeling ready to beat your stress and trauma, and also to improve your health, check out my course The Foundations of Health.
If you would like to get in touch to organise nutrient deficiency testing or discuss how to address your on-going issues, please drop me a line here.
I am also working to provide as many resources as I can to support as many people as possible to be symptom free with a great quality of life, and my free downloads are a great place to start!